You have tried every antihistamine on the pharmacy shelf. You have switched brands, tried different doses, moved from tablets to nasal sprays, tried both at once. Some years they work reasonably well. Other years they do not seem to touch it. You are still sneezing, still streaming, still waking up with a blocked nose and a head full of fog, and you are starting to wonder whether this is just how you are now.
It is not. And the fact that antihistamines are not working well for you does not mean you are unusually sensitive or that nothing will help. It means your allergic response has moved beyond what antihistamines are designed to address. Acupuncture works on the parts of the allergic cascade that antihistamines cannot reach, which is why it is often most useful for precisely the people who have already tried everything else.
Key Takeaways- Antihistamines block one chemical receptor in a cascade involving dozens of inflammatory mediators. For people with moderate to severe allergic reactions, blocking histamine alone is not sufficient
- The allergic cascade includes substance P, vasoactive intestinal peptide (VIP), interleukins 4, 5, and 13, TRPV1 receptor activation, and neurogenic inflammation: none of these are affected by antihistamines
- With repeated seasonal exposure, the immune system can become sensitised to additional allergens and non-allergic triggers, broadening the reactive picture beyond what a single drug class can manage
- Acupuncture works across the immune, inflammatory, neural, and gut-microbiome dimensions of the allergic response simultaneously
- A 2022 systematic review of 30 trials found acupuncture outperformed conventional medication in symptom scores with fewer adverse effects
- Many patients who have not responded well to medication do respond to acupuncture, because the mechanism is different, not better or worse in every case, but different in a way that matters when one approach has hit its ceiling
You are not the problemOne of the things I see regularly working with patients across Middlesbrough and Teesside is how many people arrive having been told, implicitly or explicitly, that their hay fever should be manageable and that they are simply not managing it well. Antihistamines are presented as the solution, and when they do not work, the gap is treated as a personal failing rather than a limitation of the intervention. This post explains what is actually happening so you can make better decisions about what to try next.
What Antihistamines Can and Cannot Do
Antihistamines are well-named: they block histamine. Specifically, they occupy H1 receptors throughout the body so that when your immune system releases histamine in response to pollen, the histamine cannot bind to those receptors and trigger the familiar symptoms of sneezing, itching, and congestion.
For mild to moderate allergic reactions where histamine is the dominant driver of symptoms, this works. For more complex or severe reactions, histamine is one chemical in a cascade involving many others, and blocking it while leaving the rest of the cascade active produces only partial relief. This is not a failure of the medication as designed. Antihistamines do exactly what they are built to do. The problem is that in a significant proportion of sufferers, what they are built to do is not enough.
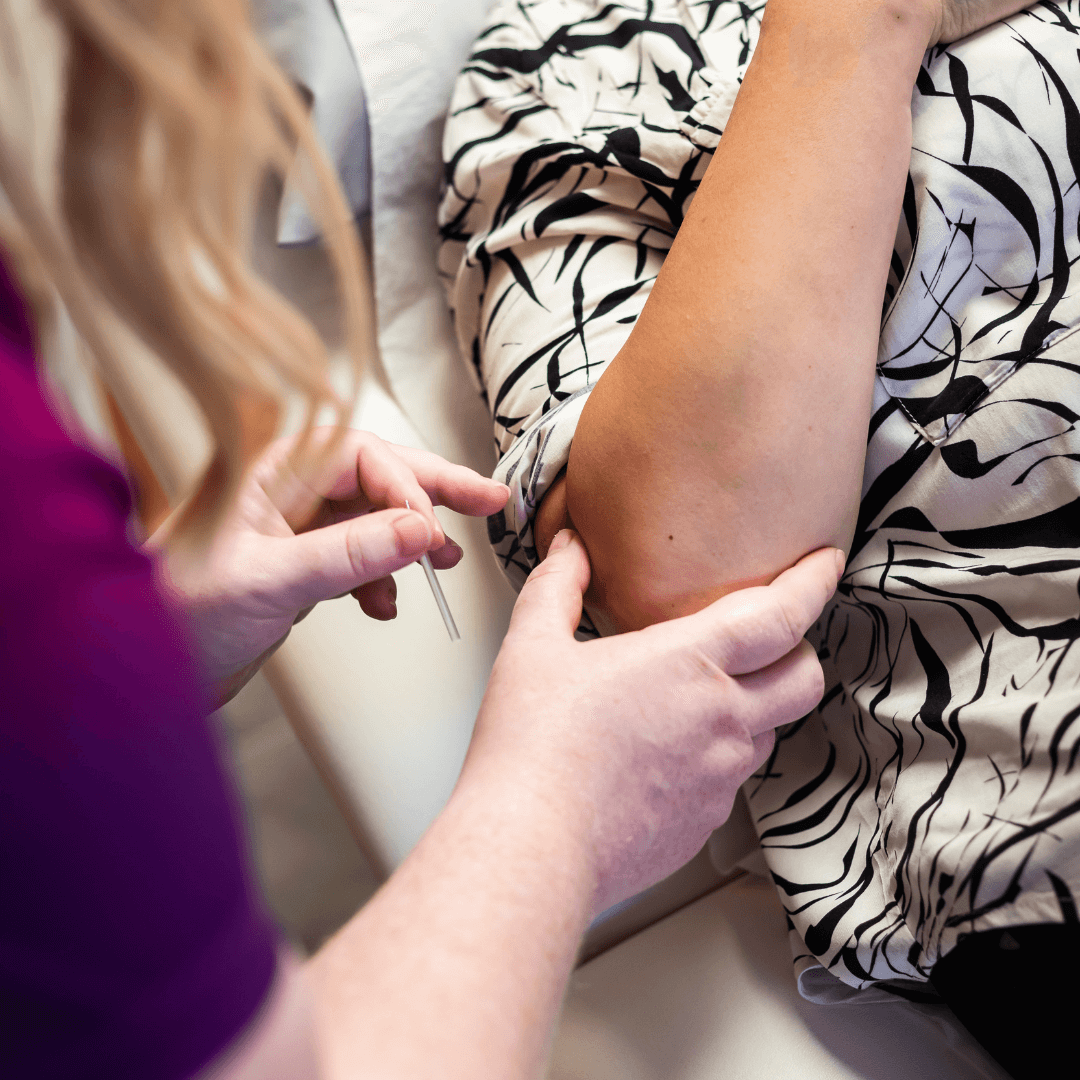 LI11 at the outer elbow is one of the most widely used anti-inflammatory points in allergy treatment. Its mechanism acts on the immune cascade rather than on a single receptor, which is why it can help when antihistamines have reached their limit.
LI11 at the outer elbow is one of the most widely used anti-inflammatory points in allergy treatment. Its mechanism acts on the immune cascade rather than on a single receptor, which is why it can help when antihistamines have reached their limit.The Allergic Cascade: What Antihistamines Miss
The allergic response is not a single event. It is a sequence of immune signalling, cell activation, inflammatory mediator release, nervous system involvement, and feedback loops that can persist and amplify over the course of an entire pollen season. Antihistamines interrupt one step. Here is what the rest of the cascade looks like, and which parts acupuncture addresses.
1
Histamine release from mast cellsIgE antibodies on the surface of mast cells bind pollen allergens, triggering immediate histamine release. This produces the rapid onset of sneezing, itching, and watery eyes within minutes of allergen exposure.
Antihistamines: partially effective here 2
Substance P and vasoactive intestinal peptide (VIP)Alongside histamine, mast cells and sensory nerves release neuropeptides including substance P and VIP. These drive nasal congestion, mucus hypersecretion, and sustained inflammation through mechanisms entirely separate from the histamine receptor pathway.
Antihistamines: no effect here 3
Pro-inflammatory cytokines (IL-4, IL-5, IL-13)The late-phase allergic response, which typically peaks 6 to 12 hours after allergen exposure, is driven by cytokines that sustain eosinophil recruitment, maintain nasal mucosal inflammation, and prolong symptoms well beyond the immediate histamine response. This is why symptoms often feel worse in the evenings or the following morning.
Antihistamines: no effect here 4
TRPV1 receptor activationThe TRPV1 receptor, found throughout the nasal mucosa and airways, is responsible for the itching and sneezing reflex. It is activated by inflammatory conditions in the nasal tissue and responds to a wide range of non-allergic triggers including temperature changes, perfume, smoke, and air quality. Once sensitised by the allergic process, it becomes a persistent driver of symptoms that persists regardless of histamine levels.
Antihistamines: no effect here 5
IgE overproduction and immune sensitisationOver repeated pollen seasons, the immune system can become sensitised to additional allergens and generate larger quantities of allergen-specific IgE. This broadens the reactive picture, increases baseline immune reactivity, and means symptoms arrive earlier, last longer, and are triggered by a wider range of environmental stimuli. Antihistamines have no effect on IgE levels.
Antihistamines: no effect here
"Antihistamines block one receptor in a response that involves dozens of mediators. For people whose allergic response has moved beyond the histamine thread, a different approach is not a last resort. It is a logical next step."
1 of 5
inflammatory mediators in the allergic cascade that antihistamines can address. The other four require a different mechanism entirely
4
distinct mechanisms acupuncture works across: immune regulation, neural modulation, inflammation control, and gut-microbiome regulation
30 RCTs
in the 2022 systematic review showing acupuncture outperformed conventional medication in symptom scores with lower adverse event rates
How Acupuncture Works Where Antihistamines Cannot
Where antihistamines occupy a single receptor type, acupuncture acts across multiple regulatory systems simultaneously. It does not simply block a different receptor: it shifts the underlying reactivity of the systems involved in the allergic response.
Mast cell regulation
Acupuncture inhibits mast cell degranulation directly, reducing the release of histamine, substance P, and VIP at the source rather than blocking receptors downstream. Less release means less total inflammatory load entering the cascade.
Cytokine rebalancing
Acupuncture downregulates the pro-inflammatory cytokines (TNF-alpha, IL-4, IL-5, IL-13) driving the late-phase response, while upregulating anti-inflammatory IL-10. This addresses the sustained inflammation that antihistamines leave untouched.
IgE reduction
Measurable reductions in total and allergen-specific IgE have been documented across multiple acupuncture studies. Lowering IgE means the mast cell response to pollen becomes less intense over time, which is the direction of true improvement rather than symptom suppression.
The Mechanism ResearchA 2025 review in the International Journal of General Medicine examined 365 studies on acupuncture's effects across allergic disorders. The researchers found that acupuncture inhibits mast cell degranulation, reduces histamine and IgE levels, and downregulates pro-inflammatory cytokines including TNF-alpha, IL-4, IL-5, and IL-13, while upregulating anti-inflammatory IL-10. Crucially, it does this through the suppression of NF-kappaB, MAPK, and TLR4/MyD88 signalling pathways, which sit upstream of the entire inflammatory cascade, not downstream of a single receptor like antihistamines.
Li Y et al., Int J Gen Med (2025) · doi.org/10.2147/IJGM.S579576
Clinical Outcomes: 30 TrialsA 2022 systematic review of 30 randomised controlled trials published in the Journal of Integrative Medicine found that acupuncture significantly outperformed conventional medication in reducing allergy symptom scores, while also displaying a lower rate of adverse events. The same review found that acupuncture reduced patients' use of rescue medication and improved quality of life outcomes. For people who have not responded adequately to antihistamines, this evidence supports acupuncture as a meaningful clinical option rather than an alternative to consider only as a last resort.
Du SH et al., J Integr Med (2022) · doi.org/10.1016/j.joim.2022.08.004
A note on this evidence: the quality of evidence for the direct comparison between acupuncture and conventional medication was rated as low by the 2022 review authors, who called for further high-quality trials. The high-confidence findings are those comparing acupuncture to sham treatment and no treatment. I will never overstate what the research currently supports. What it does support clearly is that acupuncture works significantly better than placebo, and that it operates through mechanisms that extend well beyond histamine blockade.
Why Your Symptoms May Have Got Worse Over Time
For some people, hay fever becomes more severe and harder to control over the years, not less. There are a few reasons this happens.
Repeated seasonal pollen exposure can drive progressive immune sensitisation: the immune system becomes increasingly reactive, producing larger quantities of allergen-specific IgE and responding to a wider range of triggers. What started as a mild grass pollen reaction may broaden to include tree pollen, mould, dust, and eventually non-allergic triggers like perfume or traffic fumes, as the TRPV1 pathway becomes persistently sensitised by the ongoing inflammatory environment in the nasal tissue.
There is also the question of cumulative burden. The gut microbiome, which plays a documented role in immune regulation, shifts with age, stress, antibiotics, and diet. Seasonal histamine load, especially in people with impaired DAO enzyme activity, adds to a system that is already carrying more than it was a decade ago. Antihistamines cannot address any of these compounding factors. Acupuncture, with its documented effects on the gut-microbiome and immune regulatory systems, can.
At my hay fever acupuncture clinic in Middlesbrough, some of the patients who respond most noticeably are those who have had hay fever for fifteen or twenty years and whose symptoms have steadily worsened. For these patients, addressing the accumulated pattern rather than just the seasonal surface reaction is often where the real shift happens.
Your PractitionerDeanna Thomas
BSc (Hons) Acupuncture · MBAcC · DipObsGyn · CNHC Registered
Working with patients across Middlesbrough, Yarm, and the wider Teesside area since 2021, I have built over 800 five-star reviews, many from people who had been managing hay fever with medication alone for years before trying something different.
The first appointment is always about understanding the full picture: how long you have had symptoms, how they have changed, what you have already tried, and what pattern in your system is most likely driving the picture. That is what shapes the treatment approach, not a generic allergy protocol.
Frequently Asked Questions
Do antihistamines stop working over time?
Not in the pharmacological sense of building tolerance: antihistamines do not lose their ability to block H1 receptors with repeated use. What changes is the allergic response itself. Over time and with repeated exposure, the immune system can become more broadly sensitised, produce higher levels of IgE, and drive a greater proportion of symptoms through pathways that histamine blockade cannot address. The result feels like the tablets have stopped working, but what has actually happened is that the problem has grown beyond what the tablets can cover.
Why does my hay fever seem worse some years than others?
Pollen seasons vary considerably in intensity: temperature, rainfall patterns, and air quality all affect pollen counts from year to year. But underlying immune reactivity also varies with stress levels, gut health, sleep quality, and cumulative sensitisation. A high-stress winter followed by an early, intense pollen season can produce symptoms significantly worse than the previous year even if the underlying allergy has not fundamentally changed. This year-to-year variability is one of the reasons that addressing immune regulatory capacity, not just seasonal symptoms, produces more consistent year-on-year improvement.
Is acupuncture worth trying if I have had hay fever for many years?
Yes, and possibly more so than for someone with recent-onset symptoms. Long-standing hay fever often involves a more complex and entrenched immune pattern, with broader sensitisation and higher baseline reactivity. Acupuncture's capacity to work across multiple regulatory systems simultaneously, rather than blocking a single receptor, tends to produce meaningful results in precisely this picture. I will always give an honest assessment at a first consultation based on your specific history.
Can I continue antihistamines while starting acupuncture?
Yes. Acupuncture and antihistamines work through completely different mechanisms and there is no conflict between them. Most patients I see continue their medication at the start of treatment. Many find they need it less as the season progresses and their immune reactivity reduces. I would never suggest stopping a medication without your GP's involvement. The goal is that over time you have more options and less dependence on any one of them.
How quickly does acupuncture start to work?
Most patients notice something within three to five sessions. Starting before the season peaks gives the best results, as the immune regulatory work has time to settle before your system is already in full reaction mode. Coming mid-season is still worthwhile and can reduce severity even when symptoms are already active. I always give a realistic timeline at the first consultation based on the specific picture, because the response varies between individuals and between different presentations of hay fever.
Final Thoughts
If antihistamines have been your main tool against hay fever and they are not giving you adequate control, you are not failing. You are using a tool that was designed for part of the problem and finding out that part of the problem is not all of it.
Acupuncture is not a miracle and I would never present it as one. It does not work for everyone, and I will say that clearly at a first appointment if that is my honest assessment of your situation. What it offers is a mechanism that addresses the allergic cascade at multiple levels simultaneously, in a way that accumulates benefit over time rather than requiring daily maintenance to stay ahead of symptoms.
For people who have spent years reaching for a tablet that only takes the edge off, understanding what else is available is worth the conversation. You are welcome to find out more about hay fever acupuncture in Middlesbrough, or to get in touch directly. There is no script and no pressure.
Ready to try something that works differently?
If the tablet route has hit its ceiling, there is another approach worth understanding. No obligation, no pressure.
Find Out More Just a conversation about what might help.